Choosing the right medical insurance plan can save you thousands and reduce stress during health emergencies. This guide walks you through key factors—like coverage, costs, and network—to help you make a smart, confident decision. Whether you’re self-employed or employed, understanding your options ensures you get the best care without breaking the bank.
Choosing the right medical insurance plan isn’t just about picking the cheapest option. It’s about finding a plan that fits your lifestyle, protects your finances, and gives you peace of mind when you need care the most. With so many plans available—from employer-sponsored health insurance to individual market options—it can feel overwhelming. But don’t worry. This guide breaks it down step by step so you can make an informed decision that works for you.
Medical insurance is one of the most important investments you can make in your well-being. Whether you’re young and healthy or managing a chronic condition, the right plan can mean the difference between a manageable expense and a financial crisis. In this article, we’ll walk you through everything you need to know about how to choose the right medical insurance plan—no jargon, no confusion, just clear, practical advice.
Key Takeaways
- Understand Your Needs: Start by evaluating your health history, family size, and expected medical expenses to determine what type of coverage you truly need.
- Compare Costs Carefully: Look beyond the monthly premium—consider deductibles, copays, coinsurance, and out-of-pocket maximums to understand the full financial picture.
- Check the Provider Network: Ensure your preferred doctors, hospitals, and specialists are in-network to avoid surprise bills and higher costs.
- Review Coverage Benefits: Make sure the plan covers essential services like preventive care, prescriptions, mental health, and emergency services.
- Consider Additional Riders: Think about adding dental, vision, or critical illness coverage if your base plan doesn’t include them.
- Check for Employer Contributions: If offered, take advantage of employer-sponsored plans—they often come with lower premiums and better benefits.
- Read the Fine Print: Always review the Summary of Benefits and Coverage (SBC) and Exclusions to avoid unexpected gaps in coverage.
📑 Table of Contents
- Understanding Your Health Needs and Budget
- Comparing Plan Costs: Premiums, Deductibles, and Out-of-Pocket Limits
- Evaluating Coverage and Benefits
- Checking the Provider Network
- Understanding Enrollment Periods and Special Situations
- Additional Considerations: Riders, HSAs, and Employer Plans
- Final Tips for Choosing the Right Medical Insurance Plan
Understanding Your Health Needs and Budget
Before you start comparing plans, take a moment to assess your personal health situation and financial comfort level. This foundational step will help you narrow down your options and avoid choosing a plan that doesn’t meet your real needs.
Evaluate Your Health History and Family Situation
Ask yourself: How often do you visit the doctor? Do you have a chronic condition like diabetes or hypertension? Do you have dependents—children, elderly parents, or a spouse—who rely on your insurance? If you’re generally healthy and rarely need medical care, a high-deductible plan with a Health Savings Account (HSA) might make sense. But if you have ongoing health needs, a plan with lower out-of-pocket costs could be more beneficial.
For example, Sarah, a 32-year-old freelance graphic designer, doesn’t have any chronic conditions and only visits the doctor once a year. She’s comfortable with a higher deductible because she rarely uses medical services. On the other hand, Mark, a 45-year-old father of two with asthma, needs regular inhalers and annual checkups. For him, a plan with low copays and strong prescription coverage is essential.
Set a Realistic Budget
Next, consider how much you can afford to pay monthly and out-of-pocket. Don’t just look at the premium—the monthly cost you pay to keep the plan active. Also factor in deductibles (how much you pay before insurance kicks in), copays (fixed amounts for visits or prescriptions), coinsurance (your share of costs after deductible), and out-of-pocket maximums (the most you’ll ever pay in a year).
A common mistake is choosing the plan with the lowest premium only to find that the deductible is so high you can’t afford care when you need it. For instance, a plan with a $100/month premium and a $6,000 deductible might seem cheap, but if you need surgery, you could end up paying thousands before coverage begins.
Use the Metal Tier System as a Starting Point
Most health insurance plans are categorized into metal tiers: Bronze, Silver, Gold, and Platinum. These tiers reflect how costs are split between the insurer and you.
– Bronze plans have the lowest premiums but higher out-of-pocket costs. Best for those who rarely use medical services.
– Silver plans offer a balance—moderate premiums and lower out-of-pocket costs. These are often ideal for people who qualify for subsidies.
– Gold and Platinum plans have higher premiums but significantly lower out-of-pocket expenses. Great for those with frequent medical needs.
Think of it like car insurance—choosing a plan based on how much risk you’re willing to take financially.
Comparing Plan Costs: Premiums, Deductibles, and Out-of-Pocket Limits

Visual guide about How to Choose the Right Medical Insurance Plan
Image source: medassureservices.com
When evaluating plans, it’s tempting to focus only on the monthly premium. But the real cost of a plan includes more than that. Let’s break down the key financial components.
Premiums: The Monthly Cost
This is the amount you pay each month to keep your insurance active—regardless of whether you use it. Premiums vary based on your age, location, tobacco use, and the plan you choose. For example, a 25-year-old in a rural area might pay $200/month, while a 60-year-old in a major city could pay $800/month for the same plan.
If you’re on a tight budget, you might lean toward a lower-premium plan. But remember: a low premium often means higher out-of-pocket costs when you need care.
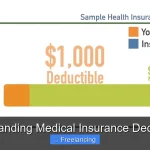
Deductibles: What You Pay Before Insurance Starts
The deductible is the amount you must pay for covered services before your insurance begins to pay. For example, if your deductible is $1,500 and you have a $1,000 doctor’s visit, you pay the full $1,000. Once you hit $1,500 in expenses, insurance starts covering its share.
Some plans have low deductibles (like $500), while others have high deductibles (like $5,000 or more). High-deductible plans are often paired with HSAs, which allow you to save pre-tax money for medical expenses.
Copays and Coinsurance: Your Share After Deductible
– Copays are fixed amounts you pay for specific services, like $30 for a doctor’s visit or $15 for a generic prescription.
– Coinsurance is a percentage you pay after meeting your deductible. For example, if your plan covers 80% of costs, you pay 20%.
These costs add up quickly, especially if you have multiple visits or medications.
Out-of-Pocket Maximum: The Most You’ll Ever Pay
This is the most you’ll pay for covered services in a year. Once you reach this limit, the insurance covers 100% of additional costs. For example, if your out-of-pocket maximum is $8,000 and you’ve already paid $7,500, the next $1,000 in expenses are fully covered.
This cap protects you from financial ruin during a major health event.
Example: Comparing Two Plans
Let’s say you’re choosing between two plans:
Plan A:
– Premium: $300/month
– Deductible: $1,000
– Copay: $25 for doctor visits
– Out-of-pocket max: $5,000
Plan B:
– Premium: $450/month
– Deductible: $300
– Copay: $15 for doctor visits
– Out-of-pocket max: $3,000
Over a year, Plan A costs $3,600 in premiums plus out-of-pocket expenses. Plan B costs $5,400 in premiums but much less in out-of-pocket costs if you use healthcare frequently. If you anticipate needing regular care, Plan B might be the better value.
Evaluating Coverage and Benefits

Visual guide about How to Choose the Right Medical Insurance Plan
Image source: weallthwisdom.com
Not all medical insurance plans are created equal when it comes to what they cover. Some include dental, vision, mental health, maternity care, or prescription drugs—others don’t. Here’s how to make sure your plan includes the services you need.
Essential Health Benefits
Under the Affordable Care Act (ACA), most individual and family plans must cover ten essential health benefits. These include:
– Ambulatory patient services (outpatient care)
– Emergency services
– Hospitalization
– Maternity and newborn care
– Mental health and substance use disorder services
– Prescription drugs
– Rehabilitative and habilitative services
– Laboratory services
– Preventive and wellness services
– Pediatric dental and vision care (for children)
Make sure your plan includes these. If it doesn’t, it’s not compliant with ACA standards.
Prescription Drug Coverage
If you take regular medications, check whether your plan includes prescription coverage and what it costs. Some plans have a formulary—a list of approved drugs—and tiered pricing. Generic drugs are usually cheaper than brand-name ones.
For example, if you take a $200/month insulin, a plan with a $10 copay for generics and a $50 copay for brand-name drugs could save you hundreds each year.
Mental Health and Substance Use Services
Mental health care is just as important as physical health. Look for plans that offer counseling, therapy, and medication management without excessive out-of-pocket costs. Some plans require prior authorization or limit the number of therapy sessions, so read carefully.
Preventive Care
Most ACA-compliant plans cover preventive services at no cost to you—like annual checkups, vaccinations, and cancer screenings. This is a huge benefit. Make sure your plan includes these without requiring a copay or deductible.
Special Needs: Chronic Conditions and Maternity Care
If you have a chronic condition like diabetes or asthma, look for a plan with strong network coverage for specialists and low copays for medications. For women planning pregnancy, maternity coverage is essential—some plans don’t include it unless you add a rider.
Checking the Provider Network

Visual guide about How to Choose the Right Medical Insurance Plan
Image source: trendydamsels.com
One of the most important factors in choosing a medical insurance plan is the provider network. This determines which doctors, hospitals, and specialists you can see without paying extra.
What Is an In-Network Provider?
In-network providers have a contract with your insurance company to offer services at negotiated rates. If you use an in-network provider, you’ll pay less out-of-pocket. Out-of-network providers cost more—sometimes significantly more.
For example, a routine MRI at an in-network hospital might cost $500, while the same scan at an out-of-network facility could cost $2,000.
How to Check Your Network
Most insurance companies have online directories where you can search for doctors and hospitals by name or location. Before choosing a plan, verify that your primary care physician, specialist, and preferred hospital are in-network.
If you travel often, consider a plan with a broad national network. If you live in a rural area, make sure the plan covers nearby facilities.
Specialist Access
Some plans require referrals to see specialists. Others let you go directly. If you see specialists regularly, a plan with no referral requirements might be more convenient—and cheaper.
Telehealth Services
Many plans now include telehealth options, allowing you to consult a doctor online for minor issues like colds, rashes, or anxiety. This is especially useful if you have a busy schedule or live in a remote area. Check whether your plan includes telehealth and how much it costs.
Understanding Enrollment Periods and Special Situations
Timing matters when signing up for medical insurance. Missing the enrollment window can leave you uninsured—or force you to pay penalties (in some states).
Open Enrollment Period
This is the annual period when you can sign up for or change your health insurance plan. For 2024, it runs from November 1 to January 15 in most states. Missing it means you’ll have to wait until the next open enrollment unless you qualify for a special circumstance.
Special Enrollment Period (SEP)
Life events like getting married, having a baby, losing job-based coverage, or moving to a new state can qualify you for a special enrollment period. These events give you 60 days to enroll in a new plan outside the regular window.
For example, if you get married in June, you can sign up for a new plan by August 15.
Medicaid and CHIP
If your income is low, you may qualify for Medicaid or the Children’s Health Insurance Program (CHIP). These government programs offer free or low-cost coverage with minimal out-of-pocket costs. Check your eligibility based on income and family size.
Marketplace Subsidies
If you buy insurance through the Health Insurance Marketplace (Healthcare.gov), you may qualify for premium tax credits or cost-sharing reductions based on income. These can lower your monthly payments or reduce out-of-pocket costs.
For example, if you earn $30,000 a year, you might qualify for a subsidy that reduces your premium by $200/month.
Additional Considerations: Riders, HSAs, and Employer Plans
Beyond the basics, there are several other factors to consider when choosing a medical insurance plan.
Health Savings Accounts (HSAs)
If you choose a high-deductible health plan (HDHP), you may be eligible to open an HSA. This is a tax-advantaged account that lets you save money for medical expenses. Contributions are tax-deductible, the money grows tax-free, and withdrawals for qualified medical expenses are tax-free.
HSAs are a powerful tool for long-term savings. For example, if you contribute $3,000 a year to an HSA and invest it wisely, you could build a medical fund over time.
Adding Riders for Extra Coverage
Some plans allow you to add riders for dental, vision, or critical illness. These aren’t always included in base plans, so consider whether you need them. For example, if you wear glasses or contacts, vision coverage could save you $200–$300 a year.
Employer-Sponsored Insurance
If your job offers health insurance, it’s usually worth considering. Employer plans often have lower premiums because the company contributes. They may also offer additional benefits like wellness programs or mental health support.
However, don’t assume it’s the best option. Compare it with individual plans on the marketplace to see which offers better value.
COBRA and Continuation Coverage
If you lose your job, you may be able to continue your employer’s plan through COBRA. This is expensive—you pay the full premium plus a 2% administrative fee—but it’s an option if you can’t immediately find new coverage.
Final Tips for Choosing the Right Medical Insurance Plan
Making the right choice takes time, but it’s worth the effort. Here are some final tips to guide you:
– Start early: Don’t wait until the last minute. Research and compare plans well before the enrollment deadline.
– Use comparison tools: Websites like Healthcare.gov, eHealth, or your state exchange allow you to compare plans side by side.
– Read reviews: Look at customer satisfaction ratings and complaint data from the National Committee for Quality Assurance (NCQA).
– Talk to a broker: If you’re confused, a licensed insurance broker can help you navigate options without charging you extra.
– Update annually: Your needs change. Re-evaluate your plan every year during open enrollment.
Remember, the best plan is one that fits your lifestyle, protects your health, and keeps your finances stable.
Frequently Asked Questions
What is the difference between a premium and a deductible?
The premium is the monthly cost you pay to keep your insurance active. The deductible is the amount you pay for covered services before your insurance starts covering costs. Think of the premium as the subscription fee, and the deductible as your out-of-pocket cost before the plan kicks in.
Can I change my medical insurance plan after enrollment?
You can only change your plan during the annual open enrollment period or if you qualify for a special enrollment period due to life events like marriage, birth, or job loss. After that, you’ll need to wait until the next enrollment window.
What is a Health Savings Account (HSA)?
An HSA is a tax-advantaged savings account linked to a high-deductible health plan. You can contribute pre-tax money, use it for qualified medical expenses, and the funds roll over year after year. It’s a great way to save for future healthcare costs.
Are all doctors covered under my insurance plan?
No. Insurance plans have networks of in-network providers who offer services at agreed-upon rates. Using out-of-network providers can result in higher out-of-pocket costs. Always check your plan’s directory before scheduling appointments.
What if I miss the open enrollment deadline?
If you miss the open enrollment period, you may remain on your current plan—but you can’t make changes unless you qualify for a special enrollment period due to qualifying life events like marriage, moving, or losing job-based coverage.
How do I know if a plan is right for me?
Consider your health needs, budget, and preferred providers. Compare premiums, deductibles, copays, and network coverage. Use comparison tools and read the Summary of Benefits and Coverage (SBC) to make an informed choice.