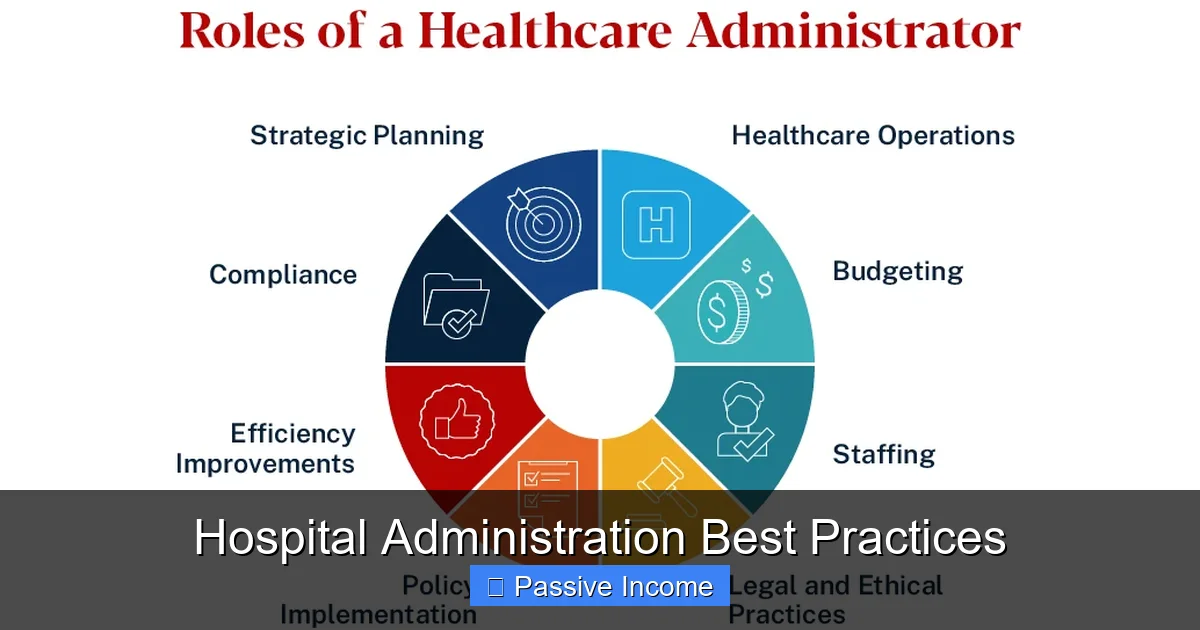
Effective hospital administration is the backbone of quality healthcare delivery and long-term financial success. By implementing hospital administration best practices, leaders can reduce costs, enhance patient satisfaction, and create scalable systems that support passive income opportunities through healthcare consulting or digital services. This guide walks you through actionable strategies to transform your hospital operations—whether you’re managing a clinic or building a healthcare-related business model.
Key Takeaways
- Patient-Centered Care Models: Prioritize patient experience through streamlined scheduling, clear communication, and empathy training for staff.
- Data-Driven Decision Making: Use real-time analytics to monitor performance, reduce waste, and improve resource allocation.
- Staff Engagement & Retention: Invest in continuous training, fair compensation, and a positive workplace culture to reduce turnover.
- Operational Efficiency: Automate routine tasks like billing, inventory, and appointment management to save time and reduce errors.
- Financial Sustainability: Diversify revenue streams—such as telehealth or outpatient services—to build passive income and financial resilience.
- Regulatory Compliance: Stay updated on healthcare laws (e.g., HIPAA) to avoid penalties and maintain trust.
- Technology Integration: Adopt EHR systems, AI tools, and mobile apps to improve coordination and scalability.
📑 Table of Contents
- Introduction: Why Hospital Administration Matters More Than Ever
- 1. Prioritize Patient-Centered Care
- 2. Leverage Data for Smarter Decisions
- 3. Invest in Your People
- 4. Automate and Optimize Operations
- 5. Build Financial Resilience
- 6. Stay Ahead of Regulations
- Conclusion: Leading with Purpose and Profit
Introduction: Why Hospital Administration Matters More Than Ever
Running a hospital isn’t just about healing patients—it’s about running a complex, high-stakes business with lives on the line. In today’s healthcare landscape, hospitals face rising costs, staffing shortages, regulatory pressures, and increasing patient expectations. That’s why hospital administration best practices aren’t just helpful—they’re essential.
When done right, effective hospital administration leads to smoother operations, happier patients, and stronger bottom lines. It’s the difference between a facility that barely survives and one that thrives. And for entrepreneurs or healthcare professionals looking to build passive income, understanding these practices opens doors to consulting, training programs, digital health products, and scalable service models.
In this article, we’ll explore proven hospital administration best practices that improve outcomes, reduce burnout, and create opportunities for sustainable growth. Whether you’re a hospital CEO, department head, or healthcare innovator, these strategies will help you lead smarter and build value—both for your organization and your personal income goals.
1. Prioritize Patient-Centered Care

Visual guide about Hospital Administration Best Practices
Image source: 0701.static.prezi.com
At the heart of every successful hospital is a simple truth: patients come first. Hospital administration best practices begin with placing the patient experience at the center of every decision.
Understanding Patient Expectations
Modern patients want more than just medical treatment—they want convenience, respect, and clear communication. They expect shorter wait times, easy access to records, and compassionate care. When hospitals fail to meet these expectations, patient satisfaction drops, and word-of-mouth suffers.
For example, a hospital that implements a patient portal where individuals can schedule appointments, view test results, and message their care team sees a 30% increase in patient satisfaction scores within six months. This kind of digital-first approach is no longer optional—it’s a competitive necessity.
Empowering Staff with Empathy Training
Even the most skilled doctors and nurses can deliver poor patient experiences if they lack bedside manner. That’s why empathy training should be a core part of hospital administration best practices.
Programs like “Healing Hands” or “Patient Communication Workshops” teach staff how to listen actively, manage difficult conversations, and show compassion—even in high-stress situations. One rural hospital in Montana reduced patient complaints by 40% after launching monthly empathy sessions led by behavioral health experts.
Streamlining the Patient Journey
A confusing patient journey leads to frustration and errors. Hospital administrators should map out every touchpoint—from check-in to discharge—and identify bottlenecks.
For instance, a hospital in Texas introduced a “one-stop check-in” kiosk system. Patients now scan their ID, verify insurance, and receive a wristband—all in under two minutes. This reduced front-desk wait times by 60% and freed up staff to focus on care coordination.
2. Leverage Data for Smarter Decisions

Visual guide about Hospital Administration Best Practices
Image source: healthcaresalaryworld.com
Gone are the days when hospital leaders relied on gut feelings to make decisions. Today, data is king—and hospital administration best practices are built on analytics.
Real-Time Performance Dashboards
Imagine being able to see how many beds are occupied, how long patients wait for lab results, or how much a department spends on supplies—all in real time. That’s the power of a centralized dashboard.
A large urban hospital in Chicago uses a custom-built dashboard to track key metrics like length of stay, readmission rates, and staff-to-patient ratios. When they noticed a spike in emergency room wait times, they reallocated staff during peak hours and added a triage nurse. Within a month, patient wait times dropped by 25%.
Predictive Analytics for Resource Planning
Predictive analytics can forecast patient admissions, disease outbreaks, or supply shortages. For example, a hospital in Florida used weather data and historical trends to predict flu season surges. They pre-positioned extra staff and supplies, avoiding overcrowding and stockouts.
This kind of proactive planning isn’t just efficient—it’s cost-saving. Hospitals that use predictive analytics report an average 15% reduction in operational costs.
Data Security and Privacy
With great data comes great responsibility. Hospital administrators must ensure patient information is protected under HIPAA and other regulations. Regular audits, staff training, and encrypted systems are non-negotiable.
A breach can cost millions in fines and damage trust. But when data is used ethically and securely, it becomes a powerful tool for improving care and driving innovation.
3. Invest in Your People

Visual guide about Hospital Administration Best Practices
Image source: entri.app
Your staff are your greatest asset—and your biggest challenge. Hospital administration best practices focus heavily on human capital because no system works without engaged employees.
Recruitment and Onboarding
Hiring the right people is only half the battle. The other half is helping them succeed from day one. A well-designed onboarding program—covering hospital culture, EHR systems, and emergency protocols—can reduce new hire turnover by 30%.
For example, a hospital in Oregon pairs new nurses with “buddy nurses” for their first 90 days. This peer mentorship model improved confidence, reduced errors, and increased retention.
Continuous Learning and Development
Healthcare evolves fast. Hospitals must offer ongoing training in new technologies, treatments, and soft skills. Online learning platforms like Coursera or internal microlearning apps make it easy for staff to learn at their own pace.
One hospital in Ohio launched a “Skills Passport” program, where employees earn digital badges for completing training modules. These badges are tied to promotions and bonuses, creating a culture of growth.
Recognition and Rewards
People stay where they feel valued. Hospital administration best practices include regular recognition—whether it’s “Employee of the Month” awards, shout-outs in team meetings, or profit-sharing plans.
A hospital in Arizona introduced a peer-nominated “Star Performer” program. Employees can give each other points redeemable for gift cards or extra PTO. Within a year, staff morale improved, and overtime hours dropped.
4. Automate and Optimize Operations
Time is money—and in healthcare, wasted time is often wasted lives. Hospital administration best practices rely on automation to eliminate inefficiencies.
Electronic Health Records (EHR)
EHR systems replace paper charts and scattered files. They allow doctors to access patient histories instantly, reduce duplication of tests, and improve care coordination.
But EHRs only work well if they’re user-friendly. One hospital in Indiana found that staff spent 30% of their time navigating the system. After switching to a simpler interface, they saved 10 hours per week per doctor—time that could be spent with patients.
Automated Billing and Coding
Billing errors are costly and stressful. Automated systems can reduce claim denials by catching coding mistakes before submission.
A hospital in Nevada used AI-powered coding software and saw a 20% increase in first-pass claim acceptance. This meant faster payments and fewer follow-ups with insurance companies.
Inventory Management Systems
Hospitals waste millions annually on expired drugs, unused supplies, and overstocking. Smart inventory systems track usage patterns, send reorder alerts, and integrate with suppliers.
A children’s hospital in Denver implemented a barcode scanning system for medical supplies. They reduced waste by 18% and saved $400,000 in one year.
5. Build Financial Resilience
Healthcare is expensive to run—and even more expensive to fail. Hospital administration best practices include strategies to ensure long-term financial health.
Diversify Revenue Streams
Relying solely on patient fees is risky. Hospitals that offer telehealth, outpatient surgery, or wellness programs create multiple income streams.
For example, a rural clinic in Wyoming started offering virtual consultations. They now earn $150,000 annually from telehealth—a sustainable passive income with minimal overhead.
Negotiate with Insurers
Insurance contracts can make or break a hospital’s finances. Administrators should negotiate favorable rates and understand reimbursement rules.
A hospital in Florida renegotiated its contract with a major insurer and increased reimbursement rates by 12%. The savings were reinvested into patient care and staff training.
Monitor Key Financial Metrics
Track metrics like operating margin, cost per case, and days in accounts receivable. These indicators help identify financial weaknesses early.
A hospital in Ohio used financial dashboards to spot a rising cost per case in its cardiology department. After auditing procedures, they found redundant tests. Cutting those tests saved $750,000 annually.
6. Stay Ahead of Regulations
Healthcare is one of the most regulated industries. Hospital administration best practices include proactive compliance to avoid fines, lawsuits, and reputational damage.
Regular Compliance Audits
Conduct internal audits quarterly to check for HIPAA violations, OSHA safety issues, and billing inaccuracies.
A hospital in California avoided a $2 million HIPAA penalty by catching a data breach early through routine audits. They fixed the issue and updated their security protocols.
Staff Training on Compliance
Employees must understand their role in compliance. Annual training on privacy, safety, and ethics should be mandatory.
A hospital in Texas saw a 50% drop in compliance incidents after launching interactive online training modules with quizzes and real-life scenarios.
Stay Updated on Policy Changes
Healthcare laws change often. Subscribe to government alerts, join industry associations, and attend conferences to stay informed.
A hospital administrator in Nevada used a policy tracking tool to anticipate changes in Medicaid reimbursement. They adjusted their billing strategy six months early, avoiding revenue loss.
Conclusion: Leading with Purpose and Profit
Hospital administration best practices aren’t just about running a smooth operation—they’re about creating a sustainable, compassionate, and profitable healthcare environment. When hospitals focus on patients, empower staff, embrace technology, and manage finances wisely, they lay the foundation for long-term success.
For healthcare professionals and entrepreneurs, these practices also open doors to passive income opportunities. Whether you’re building a training course on hospital leadership, launching a telehealth platform, or offering consulting services, understanding how top hospitals operate gives you a competitive edge.
The future of healthcare belongs to those who lead with empathy, data, and innovation. By applying these best practices, you’re not just improving patient care—you’re building a legacy and creating value that lasts.
Frequently Asked Questions
What are the most important hospital administration best practices?
Key practices include prioritizing patient-centered care, using data for decision-making, investing in staff, automating operations, ensuring financial resilience, and maintaining regulatory compliance. These strategies improve care quality, reduce costs, and support long-term sustainability.
How can hospital administration create passive income?
Hospital administrators can generate passive income through consulting, digital health products (like apps or courses), telehealth services, or partnerships with medical device companies. By leveraging expertise in operations and compliance, they can build scalable revenue streams outside traditional employment.
What role does technology play in hospital administration?
Technology improves efficiency, accuracy, and patient outcomes. Tools like EHRs, AI analytics, and automated billing reduce errors and save time. When integrated thoughtfully, they become a force multiplier for hospital administrators.
How can small hospitals apply these best practices?
Small hospitals can start small—implementing patient portals, staff training programs, or basic inventory tracking. Even low-cost or free tools (like Google Forms for feedback or Excel for dashboards) can yield big results. Focus on one area at a time and scale as resources allow.
Why is staff engagement critical in hospital administration?
Engaged staff are more productive, make fewer errors, and stay longer. High turnover increases training costs and disrupts patient care. Hospital administration best practices that prioritize recognition, development, and fair compensation lead to a stronger, more resilient workforce.
Can hospital administration practices be applied outside hospitals?
Absolutely. Many principles—like data-driven decisions, patient experience, and operational efficiency—apply to clinics, nursing homes, urgent care centers, and even health-tech startups. Hospital administration best practices are transferable across healthcare settings.