How doctors decide hospital treatment options involves a careful process of gathering information, analyzing symptoms, and reviewing test results. They consider your medical history, current condition, and potential risks before choosing the best course of action. This decision-making process ensures that patients receive personalized, effective care tailored to their unique needs.
Key Takeaways
- Patient History Matters: Doctors review past illnesses, medications, and family health to understand what might be influencing your current condition.
- Clinical Guidelines Guide Decisions: Treatment choices are often based on established medical guidelines that reflect the latest research and best practices.
- Diagnostic Tests Inform Plans: Blood work, imaging, and other tests help doctors pinpoint the cause of symptoms and determine the most effective treatment.
- Team Collaboration Is Key: In complex cases, doctors consult specialists, nurses, and other healthcare providers to reach a well-rounded decision.
- Risk vs. Benefit Analysis: Every treatment option is weighed against potential risks, side effects, and expected outcomes to minimize harm.
- Patient Preferences Are Considered: Doctors discuss options with patients, respecting their values, lifestyle, and goals when making treatment plans.
- Continuous Monitoring Adjusts Care: Treatment plans are not static—they’re updated based on how the patient responds and new information becomes available.
📑 Table of Contents
- How Doctors Decide Hospital Treatment Options
- Step 1: Initial Assessment and Triage
- Step 2: Gathering and Analyzing Medical Information
- Step 3: Diagnosis and Differential Diagnosis
- Step 4: Choosing Treatment Options
- Step 5: Consulting with a Medical Team
- Step 6: Implementing and Monitoring Treatment
- Step 7: Discharge Planning and Follow-Up
- How Patients Can Support the Decision-Making Process
- Common Challenges in Treatment Decision-Making
- Technology and Data in Treatment Decisions
- Conclusion
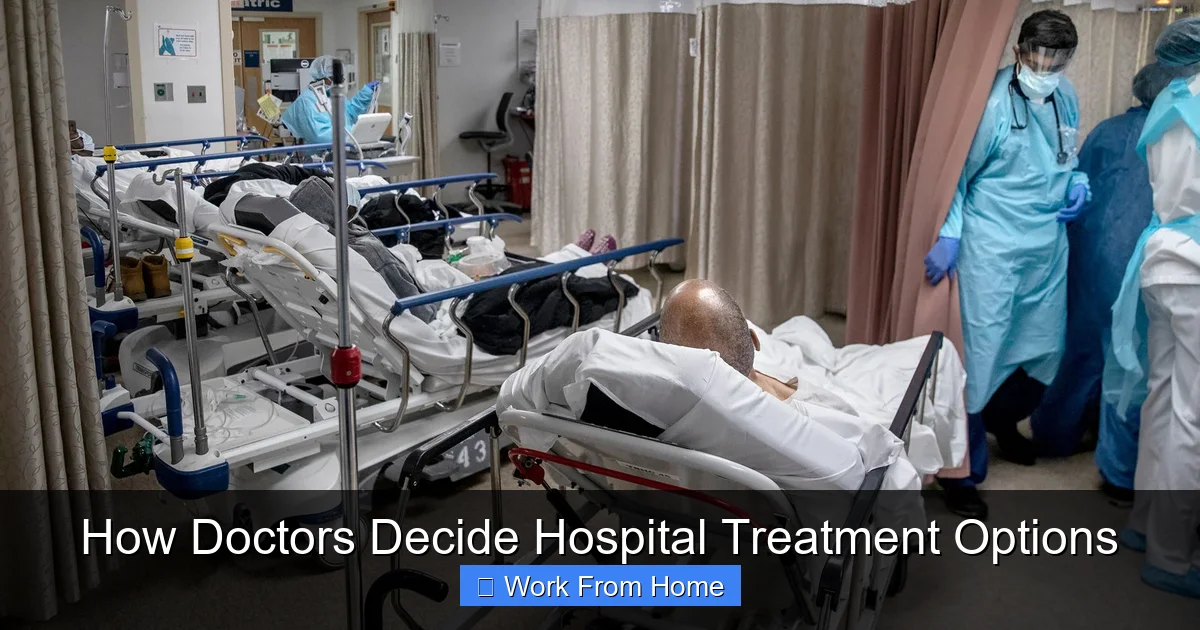
How Doctors Decide Hospital Treatment Options
Have you ever wondered what goes on behind the scenes when a doctor decides how to treat you in the hospital? It’s not just about flipping through a checklist or following a routine. Behind every treatment decision lies a thoughtful, evidence-based process shaped by science, experience, and compassion. Whether you’re dealing with a broken bone, a severe infection, or a complex chronic condition, understanding how doctors make treatment choices can help you feel more informed and confident about your care.
In this article, we’ll walk you through the step-by-step process doctors use to decide on hospital treatment options. From the moment you arrive at the emergency room to the moment you’re discharged, your care is guided by clinical reasoning—a blend of observation, data, and judgment. We’ll explore how doctors gather information, weigh risks, consult with colleagues, and tailor treatments to each patient’s unique situation. By the end, you’ll have a clearer picture of how medical decisions are made and what you can do to support the process.
Step 1: Initial Assessment and Triage
When you first arrive at the hospital, whether by ambulance or walk-in, the first step is a rapid assessment. This is often done by triage nurses or emergency room doctors who evaluate your symptoms, vital signs (like blood pressure, heart rate, and temperature), and overall condition. The goal is to determine how urgent your situation is.

Visual guide about How Doctors Decide Hospital Treatment Options
Image source: i.dailymail.co.uk
What Happens During Triage?
Triage helps prioritize patients based on the severity of their condition. For example, someone having a heart attack will be seen before someone with a minor cut. During this phase, doctors ask key questions:
- What symptoms are you experiencing?
- When did they start?
- How severe are they on a scale of 1 to 10?
- Do you have any known medical conditions?
This initial evaluation sets the stage for everything that follows. It helps doctors decide how quickly you need to be seen and what tests or interventions might be needed first.
Why It Matters
Even before a full diagnosis is made, the triage process influences treatment decisions. For instance, if you’re showing signs of sepsis (a life-threatening response to infection), doctors will begin treatment immediately—even before all test results are back. This is an example of how urgency and clinical judgment shape early care.
Step 2: Gathering and Analyzing Medical Information
Once you’re in the care of a treating physician, the next phase begins: collecting detailed medical information. This includes your medical history, physical exam findings, and diagnostic test results.

Visual guide about How Doctors Decide Hospital Treatment Options
Image source: thumbs.dreamstime.com
Medical History Review
Doctors start by asking about your past health. This includes:
- Previous surgeries or hospitalizations
- Chronic conditions like diabetes, hypertension, or asthma
- Current medications (including over-the-counter drugs and supplements)
- Family history of diseases (e.g., heart disease, cancer)
- Allergies
This information helps doctors understand what might be contributing to your current symptoms and avoid treatments that could interact with existing conditions.
Physical Examination
A hands-on exam allows doctors to observe signs of illness. For example:
- A swollen, red knee might suggest an infection or injury.
- Lung sounds that are too quiet could indicate pneumonia.
- Abdominal tenderness might point to appendicitis.
These observations, combined with your reported symptoms, form a picture of your health that guides further testing.
Diagnostic Testing
Depending on your symptoms, doctors may order tests such as:
- Blood tests: To check for infection, organ function, or hormone levels.
- Imaging: X-rays, CT scans, or MRIs to visualize internal structures.
- Urinalysis: To detect urinary tract infections or kidney problems.
- Electrocardiogram (ECG): To assess heart rhythm.
These tests provide objective data that help confirm or rule out possible diagnoses. For example, a chest X-ray might reveal fluid in the lungs, suggesting heart failure, while a negative result might lead doctors to consider other causes like pneumonia.
Step 3: Diagnosis and Differential Diagnosis
After gathering all the information, doctors work to identify the most likely cause of your symptoms. This process is called diagnosis, but it often starts with something called differential diagnosis.

Visual guide about How Doctors Decide Hospital Treatment Options
Image source: fournews-assets-prod-s3-ew1-nmprod.s3.amazonaws.com
What Is Differential Diagnosis?
Differential diagnosis is the process of distinguishing between possible conditions that could explain your symptoms. Doctors don’t jump to conclusions—they consider multiple possibilities and systematically rule them out.
For example, if you have chest pain, doctors might consider:
- Heart attack
- Pulmonary embolism (blood clot in the lung)
- Gastroesophageal reflux disease (GERD)
- Pneumonia
- Costochondritis (inflammation of rib cartilage)
Each of these causes different treatments, so getting the right diagnosis is critical. Doctors use test results, patient history, and clinical expertise to narrow down the list.
How Is a Diagnosis Made?
A diagnosis is typically confirmed when test results or physical findings match a known disease pattern. For instance, an elevated troponin level in blood tests is a strong indicator of a heart attack. Once a diagnosis is made, doctors can choose the most appropriate treatment.
Step 4: Choosing Treatment Options
With a diagnosis in hand, doctors begin evaluating treatment options. This is where clinical guidelines, experience, and patient factors all come into play.
Clinical Guidelines and Evidence-Based Medicine
Most hospitals follow clinical guidelines—recommendations developed by medical organizations based on research and expert consensus. For example, the American Heart Association has specific protocols for treating heart attacks, including the use of clot-busting drugs or angioplasty.
These guidelines help ensure that treatments are safe, effective, and consistent across providers. However, they’re not rigid rules. Doctors adapt them to fit individual patients.
Weighing Risks and Benefits
Every treatment has potential benefits and risks. For example:
- Antibiotics: Can cure infections but may cause side effects like nausea or allergic reactions.
- Surgery: May relieve symptoms but carries risks of bleeding, infection, or anesthesia complications.
- Medications: Can manage symptoms but may interact with other drugs.
Doctors use something called a risk-benefit analysis to decide which treatment offers the best outcome with the least harm. They consider factors like your age, overall health, and how serious your condition is.
Personalizing Treatment Plans
No two patients are exactly alike. That’s why treatment plans are personalized. For instance:
- A 70-year-old with heart disease might not be a good candidate for a high-risk procedure.
- A young athlete with a torn ligament might prioritize faster recovery, even if it means a longer rehab process.
Doctors take into account your lifestyle, preferences, and goals when designing a treatment plan.
Step 5: Consulting with a Medical Team
For complex cases, doctors don’t work in isolation. They consult with a team of healthcare professionals to make the best decision.
Multidisciplinary Teams
In hospitals, teams often include:
- Specialists: Doctors with advanced training in specific areas (e.g., cardiologists, neurologists).
- Nurses: Provide ongoing monitoring and support.
- Pharmacists: Review medications for safety and interactions.
- Therapists: Help with physical, occupational, or speech therapy.
- Social workers: Assist with discharge planning or emotional support.
For example, a patient with a brain tumor might have a neurosurgeon, oncologist, radiologist, and rehabilitation specialist all involved in their care.
Second Opinions and Tumor Boards
In cancer care, doctors often participate in tumor boards—meetings where multiple specialists review a patient’s case and recommend treatment. This collaborative approach reduces the chance of oversight and improves outcomes.
Step 6: Implementing and Monitoring Treatment
Once a treatment plan is chosen, it’s put into action—but the process doesn’t end there.
Starting Treatment
Treatment might begin immediately (e.g., administering insulin for diabetic ketoacidosis) or be scheduled (e.g., surgery next week). Doctors communicate clearly with patients and families about what to expect.
Ongoing Monitoring
Patients are closely monitored for response and side effects. For example:
- Blood sugar levels are checked frequently in diabetic patients on insulin.
- CT scans are repeated to see if a tumor is shrinking.
- Medication dosages are adjusted based on lab results.
If a treatment isn’t working or is causing harm, doctors may change the plan. Flexibility is key in hospital care.
Step 7: Discharge Planning and Follow-Up
As you recover, doctors begin planning your discharge. This includes:
- Medication instructions
- Follow-up appointments
- Rehabilitation needs
- Home care requirements
Discharge isn’t just about leaving the hospital—it’s about ensuring you can manage your condition safely at home. Doctors coordinate with primary care providers and community services to support your recovery.
How Patients Can Support the Decision-Making Process
While doctors lead treatment decisions, patients play a vital role too. Here’s how you can help:
- Be honest about your symptoms: Describe pain levels, duration, and any changes.
- Bring a list of medications: Include dosages and reasons for use.
- Ask questions: If you don’t understand a test or treatment, ask for clarification.
- Share your preferences: Let doctors know if you’re hesitant about surgery or want to explore alternatives.
- Keep records: Track symptoms, test results, and treatment responses.
When you’re an active participant, treatment decisions become more effective and aligned with your goals.
Common Challenges in Treatment Decision-Making
Even experienced doctors face challenges. Here are a few:
- Unclear diagnoses: Some symptoms overlap across diseases, making it hard to pinpoint the cause.
- Limited time: In busy hospitals, doctors may have less time to discuss options in depth.
- Resource constraints: Not all hospitals have access to the latest technology or specialists.
- Patient anxiety: Fear or confusion can make it hard to communicate effectively.
Despite these challenges, doctors use tools like decision aids, electronic health records, and team huddles to improve accuracy and efficiency.
Technology and Data in Treatment Decisions
Modern hospitals use technology to support clinical reasoning. For example:
- Electronic Health Records (EHRs): Store all your medical data in one place, making it easy for providers to access.
- AI and Machine Learning: Can analyze large datasets to predict outcomes or suggest treatment options.
- Telemedicine: Allows specialists to consult remotely, expanding access to expert care.
These tools help doctors make faster, more accurate decisions—but they don’t replace human judgment.
Conclusion
How doctors decide hospital treatment options is a dynamic, multi-step process that blends science, experience, and empathy. From the initial triage to discharge planning, every decision is guided by your unique health needs and the best available evidence. While the system isn’t perfect, it’s designed to prioritize your safety and well-being.
By understanding this process, you can feel more empowered during your hospital stay. Ask questions, share your concerns, and don’t hesitate to seek clarification. When you’re informed and involved, treatment decisions become a shared journey—one that leads to better outcomes and faster recovery.
Frequently Asked Questions
How do doctors choose between different treatment options?
Doctors evaluate each treatment based on effectiveness, risks, side effects, and how well it fits the patient’s condition. They use clinical guidelines and consult with specialists to make balanced decisions.
Can patients influence treatment decisions?
Yes, absolutely. Doctors consider patient preferences, lifestyle, and goals. Open communication helps ensure the chosen treatment aligns with what matters most to the patient.
What role do medical tests play in treatment decisions?
Tests provide objective data that help confirm diagnoses and guide treatment. For example, a positive blood test for a specific marker can lead to targeted therapy.
How do doctors handle uncertainty in diagnosis?
Doctors use differential diagnosis—a process of considering and ruling out possible conditions. They may also repeat tests, seek second opinions, or try treatments that help clarify the diagnosis.
Are treatment decisions the same for every patient?
No. Even with the same diagnosis, treatment plans are personalized based on age, health status, preferences, and other individual factors.
What happens if a treatment isn’t working?
Doctors monitor progress closely. If a treatment isn’t effective or causes harm, they adjust the plan—possibly switching medications, adding therapies, or considering surgery.