Medical insurance premiums are the monthly costs you pay for coverage, and they’re calculated using a mix of personal, geographic, and policy-specific factors. Insurers look at your age, health history, location, and even lifestyle choices to determine your rate. Understanding how premiums are set can help you shop smarter and save on healthcare costs.
Key Takeaways
- Age and Gender: Younger individuals typically pay less, while older applicants face higher premiums due to increased healthcare needs.
- Geographic Location: Premiums vary by state or region due to differences in healthcare costs, provider availability, and state regulations.
- Health Status: Insurers assess pre-existing conditions and overall health to estimate future claims, impacting premium levels.
- Coverage Level: The type of plan—bronze, silver, gold, or platinum—affects how much you pay monthly and out-of-pocket.
- Deductible and Co-pays: Higher deductibles usually mean lower premiums, but more out-of-pocket costs when you need care.
- Lifestyle Factors: Smoking, BMI, and chronic conditions can increase premiums due to higher risk profiles.
- Family vs. Individual Plans: Family coverage costs more than individual plans, but the per-person cost may be lower with dependents.
📑 Table of Contents
- Medical Insurance Premiums: How They Are Calculated
- What Is a Medical Insurance Premium?
- The Core Components of Premium Calculation
- How Insurers Use Risk Assessment Models
- Examples: How Premiums Are Calculated in Real Life
- Tips to Lower Your Medical Insurance Premiums
- Conclusion: Take Control of Your Healthcare Costs
Medical Insurance Premiums: How They Are Calculated
Let’s face it—medical insurance can feel like one of those things you wish you’d never have to think about… until you do. Then suddenly, those monthly bills start rolling in, and you’re left wondering, “How did I end up paying so much?” The truth is, medical insurance premiums aren’t arbitrary numbers. They’re carefully calculated based on a variety of factors, and understanding how that works can make a huge difference in how much you spend—and how well your coverage fits your life.
Whether you’re self-employed, freelancing, or just trying to make sense of your employer-sponsored plan, knowing how premiums are set helps you shop smarter, negotiate better, and even save money. In this article, we’ll break down the science behind medical insurance pricing, explain the key factors that influence your monthly costs, and offer practical tips to keep your premiums manageable—without sacrificing coverage.
What Is a Medical Insurance Premium?
Before diving into the math, let’s clarify what a premium actually is. Think of it as your monthly subscription fee to stay covered. You pay it every month (or sometimes quarterly or annually), and in return, your insurance company agrees to help cover your medical expenses—up to the limits of your plan.

Visual guide about Medical Insurance Premiums: How They Are Calculated
Image source: i.ytimg.com
It’s important to remember that the premium is just one part of your healthcare costs. You’ll also face deductibles, co-pays, co-insurance, and out-of-pocket maximums. But the premium is the foundation—the recurring cost that keeps your coverage active. Without it, your insurance stops working, no matter how much money you’ve already spent.
The Core Components of Premium Calculation
Insurance companies don’t just guess your premium. They use a combination of actuarial data, risk assessment models, and regulatory guidelines to determine how much you should pay. This process is called risk pooling, and it’s designed to balance costs across a large group of people so that healthy individuals help cover the expenses of those who need more care.
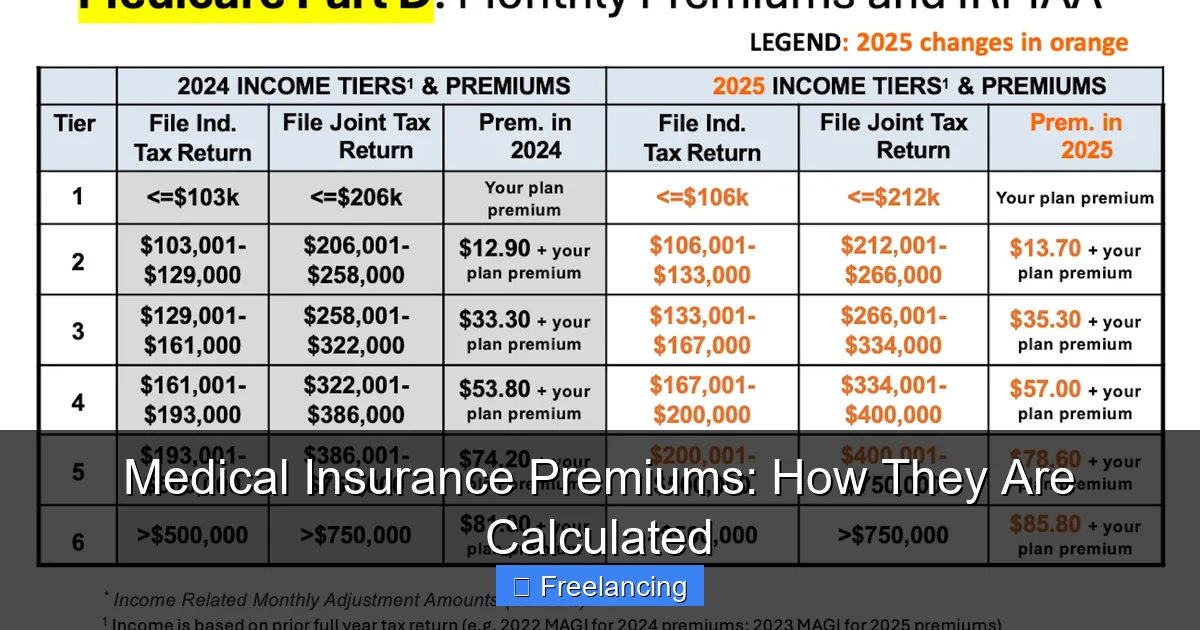

Visual guide about Medical Insurance Premiums: How They Are Calculated
Image source: senior-advisors.com
But how do they decide what your piece of that pool should be? Let’s explore the main ingredients in the premium recipe.
1. Demographic Factors: Age, Gender, and More
Your personal profile plays a big role. Age is one of the most significant factors. Why? Because older people use more healthcare services—more doctor visits, prescriptions, tests, and hospital stays. As a result, insurers charge higher premiums to older adults.
For example, a 25-year-old might pay $150/month for a basic plan, while a 65-year-old could pay $400 or more, depending on the coverage level. This difference isn’t arbitrary—it reflects real-world data showing that healthcare usage increases with age.
Gender can also matter, though this varies by region and plan type. In some countries, women pay more due to higher utilization of maternity care and preventive services. In others, men may face higher rates because of lifestyle-related risks like smoking or risky behaviors. But in the U.S., the Affordable Care Act (ACA) prohibits gender-based pricing in most individual market plans—so gender is less of a factor now than it once was.
2. Geographic Location: Where You Live Matters
Where you live can dramatically affect your premium. Healthcare costs vary widely across states and even neighborhoods. A simple MRI in New York City might cost $2,000, while the same scan in rural Kansas could be $800. Insurers factor in these regional differences when setting rates.
Additionally, some states have more competitive insurance markets, which can drive prices down. Others have fewer insurers, leading to higher premiums. For instance, California and New York often have lower average premiums due to strong regulatory oversight and large risk pools. Meanwhile, states like Alaska and Wyoming may see higher costs due to lower population density and fewer providers.
Also, state-specific regulations play a role. Some states require insurers to cover certain services (like mental health or maternity care), which can increase overall costs and, in turn, premiums.
3. Health Status and Medical History
This is where things get personal. Insurers look at your health history—especially pre-existing conditions—to estimate how much care you might need in the future. If you have diabetes, asthma, or a history of heart disease, you’re considered higher risk, and your premium may reflect that.
However, thanks to the ACA, insurers can no longer deny coverage or charge more based on pre-existing conditions in the individual market. That means your health status won’t directly increase your premium if you’re buying a plan through the Health Insurance Marketplace. But it can still influence the overall cost of care, which affects pricing across the board.
That said, if you’re on a group plan through your employer, your health status is generally not a factor. Employers negotiate rates for their entire workforce, so everyone pays the same premium regardless of individual health.
4. Type of Plan and Coverage Level
Not all insurance plans are created equal. In the ACA marketplace, plans are categorized into four metal tiers: Bronze, Silver, Gold, and Platinum. Each tier offers different levels of cost-sharing and premium amounts.
- Bronze plans have the lowest premiums but the highest out-of-pocket costs. You pay more when you get care.
- Platinum plans have the highest premiums but the lowest out-of-pocket costs. You pay less when you use services.
- Silver plans are the most popular, especially if you qualify for cost-sharing reductions. They balance premiums and out-of-pocket costs.
- Gold plans sit in the middle—higher premiums than Silver, lower than Platinum, with moderate out-of-pocket costs.
So, if you choose a Gold plan instead of a Bronze one, your premium will be higher—but you’ll spend less when you actually need medical care. This trade-off is central to how premiums are structured.
5. Deductible, Co-pays, and Co-insurance
The deductible is the amount you pay out-of-pocket before your insurance kicks in. Plans with higher deductibles usually have lower premiums, while those with low deductibles cost more upfront.
For example, a plan with a $1,000 deductible might have a $200 monthly premium. The same coverage with a $500 deductible could cost $350/month. The difference? The insurer takes on more risk early in the year, so they charge more to compensate.
Co-pays (fixed amounts you pay per visit) and co-insurance (a percentage of costs you cover) also affect pricing. Plans with low co-pays (like $20 per doctor visit) cost more than those with $50 co-pays, because insurers pay more frequently.
6. Lifestyle and Risk Factors
Believe it or not, your lifestyle can impact your premium. Insurers may consider factors like smoking, obesity, or chronic stress—though this is more common in employer-sponsored plans or private insurers than in ACA-compliant individual plans.
For instance, smokers often pay higher premiums because they use more healthcare services over time. Similarly, individuals with high BMI (Body Mass Index) or a history of substance abuse may face higher rates due to increased risk of conditions like heart disease or diabetes.
However, it’s worth noting that many insurers are moving away from penalizing healthy behaviors. Some now offer wellness incentives—like discounts for quitting smoking or completing health screenings—to encourage better outcomes.
7. Family Size and Coverage Type
If you’re covering your family, your premium will be higher than an individual plan. But it’s not always a linear increase. Some insurers offer a “family cap,” where the total premium for a family of four is less than four times the individual rate.
For example, an individual plan might cost $300/month, while a family of four could pay $900—not $1,200. This helps keep costs manageable for families while still covering multiple lives.
Also, if you add a spouse and two children, your premium will depend on whether you choose a family plan or individual plans for each person. Family plans are usually more cost-effective per person but require everyone to be on the same policy.
How Insurers Use Risk Assessment Models
Behind the scenes, insurers use complex algorithms and actuarial tables to predict how much care you’ll need. These models look at millions of data points—age, zip code, medical history, prescription use, and even hospital visit patterns—to estimate your risk level.
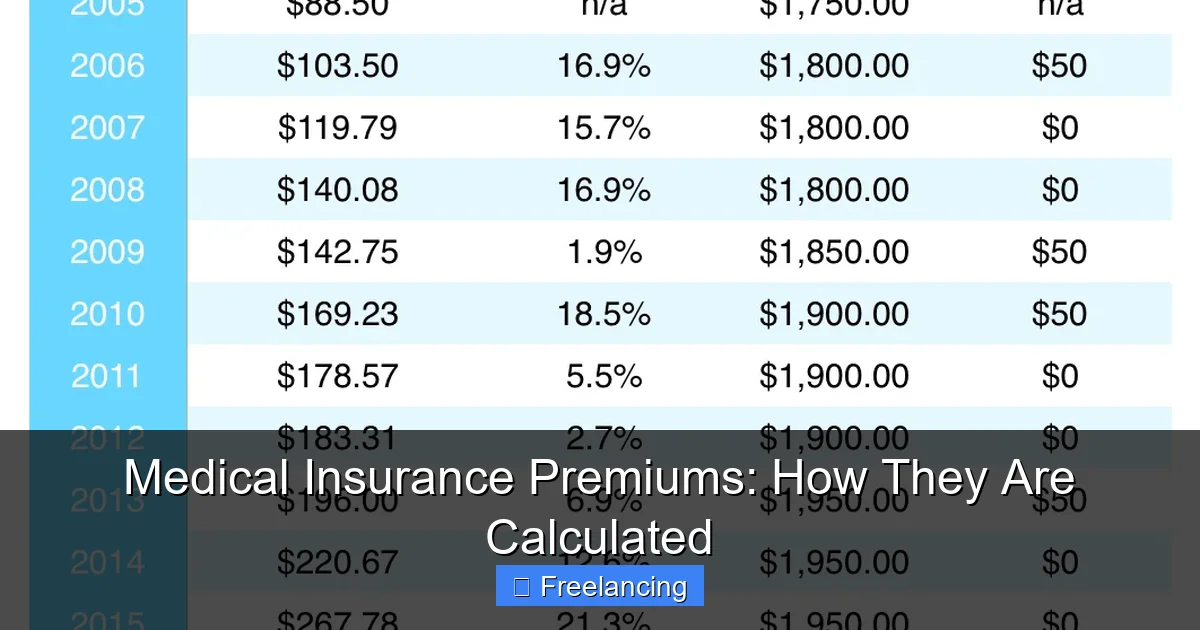
Visual guide about Medical Insurance Premiums: How They Are Calculated
Image source: pc.net
For example, if 10,000 people in your age group and region use an average of $5,000 in medical services per year, the insurer knows they need to collect enough in premiums to cover that cost—plus administrative fees and profit.
They also consider community rating rules, which require all people in a given area to pay similar rates, regardless of individual risk. This helps protect high-risk individuals from being priced out of coverage. But it also means healthier people subsidize those who need more care.
This balance is why premiums are often higher in areas with older populations or higher chronic disease rates—even if you personally are in great health.
Examples: How Premiums Are Calculated in Real Life
Let’s look at a practical example. Meet Sarah, a 32-year-old freelance graphic designer living in Austin, Texas. She’s single, in good health, and wants a Silver plan with a $2,000 deductible.
Based on current market data, here’s how her premium might break down:
- Base premium for a 32-year-old in Texas: $280/month
- Silver plan adjustment: +$40 (Silver plans are more expensive than Bronze)
- Regional cost factor: +$20 (Austin has higher healthcare costs than rural areas)
- No pre-existing conditions: No additional charge
- No lifestyle risks (non-smoker, healthy BMI): No surcharge
- Base premium for 58-year-old: $420/month
- Gold plan adjustment: +$60
- Regional factor: +$10 (Detroit is slightly above average)
- Pre-existing condition: +$25 (still allowed in ACA plans, but affects overall risk pool)
Total estimated premium: $340/month
Now compare that to Mark, a 58-year-old teacher in Detroit with diabetes, who wants a Gold plan:
Total estimated premium: $515/month
Even though both want similar coverage levels, Mark pays significantly more—not because he’s “unhealthy,” but because of his age and the higher cost of care in his area.
Tips to Lower Your Medical Insurance Premiums
While you can’t change your age or where you live, there are several smart strategies to reduce your premiums—especially if you’re freelancing or self-employed and choosing your own plan.
1. Shop During Open Enrollment or Special Enrollment Periods
Premiums can change yearly based on market conditions, inflation, and your personal updates (like income or family size). Always shop during Open Enrollment (usually November–December) or if you have a qualifying life event (like getting married or losing job-based coverage).
2. Compare Plans Side by Side
Don’t just look at the monthly premium. Check the deductible, co-pays, network size, and out-of-pocket maximum. A plan with a $100/month premium and a $10,000 deductible might cost you more in the long run than a $300/month plan with a $1,000 deductible.
3. Consider a Health Savings Account (HSA)
If you have a high-deductible health plan (HDHP), you can open an HSA. Contributions are tax-deductible, and you can use the funds tax-free for medical expenses. This can offset your out-of-pocket costs and effectively lower your overall healthcare spending.
4. Look into Subsidies
Low- and middle-income individuals may qualify for premium tax credits through the ACA Marketplace. These credits reduce your monthly premium—sometimes dramatically. Use the Healthcare.gov calculator to see if you’re eligible.
5. Choose a Larger Network or In-Network Providers
Plans with broader networks often cost more. If you’re willing to see in-network doctors and avoid out-of-network care, you might be able to switch to a lower-cost plan.
6. Maintain a Healthy Lifestyle
While not always reflected in premiums, staying healthy reduces your risk of expensive medical events. Regular check-ups, managing chronic conditions, and avoiding smoking can prevent costly hospitalizations down the road.
Conclusion: Take Control of Your Healthcare Costs
Medical insurance premiums are more than just a number on your bill—they’re the result of careful calculations based on your age, location, health, and choices. While you can’t control everything, understanding how premiums are set empowers you to make smarter decisions.
Whether you’re a freelancer choosing your first plan or someone trying to reduce monthly costs, knowing the factors behind pricing helps you shop with confidence. Compare plans, consider subsidies, and remember: the cheapest plan isn’t always the best. The right plan balances affordability with real-world needs.
And if you’re self-employed or freelancing, don’t forget—you may be eligible for tax deductions on your health insurance premiums. That’s one more way to keep more of your hard-earned money in your pocket.
Take charge today. Use this guide to evaluate your options, ask the right questions, and find a plan that fits your life—without breaking the bank.
Frequently Asked Questions
Can I negotiate my medical insurance premium?
Directly negotiating your premium with an insurer is rare, but you can influence it by shopping during open enrollment, qualifying for subsidies, or switching plans. Employers may also negotiate group rates on your behalf.
Do pre-existing conditions increase my premium?
In ACA-compliant plans, no—insurers can’t charge more based on pre-existing conditions. However, they still factor in overall risk when setting community rates, which affects premiums across the board.
Why do premiums vary so much between states?
Premiums differ due to healthcare costs, provider availability, state regulations, and the number of insurers competing in the market. States with more competition and oversight often have lower average rates.
Can I change my plan mid-year?
Only during Open Enrollment or if you have a qualifying life event (like marriage, birth, or job loss). Otherwise, you must wait until the next enrollment period.
Are family premiums always four times the individual rate?
Not necessarily. Some insurers offer a family cap, where the total cost for a family of four is less than four times the individual premium, making it more affordable than separate plans.
How do I know if I’m getting a fair premium?
Compare plans using tools like Healthcare.gov, check average rates in your area, and consider your expected healthcare usage. Look at both monthly costs and out-of-pocket maximums to evaluate total value.